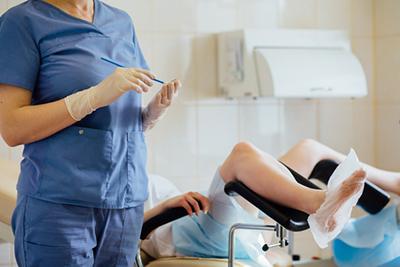
 Your reproductive system is complex, which is why you need a specialist. You need an OBGYN. The foundation of reproductive health care is routine screenings. Routine screenings can help identify
Read more
Your reproductive system is complex, which is why you need a specialist. You need an OBGYN. The foundation of reproductive health care is routine screenings. Routine screenings can help identify
Read more
posted: Apr. 16, 2024.
 Your reproductive system is complex, which is why you need a specialist. You need an OBGYN. The foundation of reproductive health care is routine screenings. Routine screenings can help identify
Read more
Your reproductive system is complex, which is why you need a specialist. You need an OBGYN. The foundation of reproductive health care is routine screenings. Routine screenings can help identify
Read more
posted: Apr. 01, 2024.
 Incontinence refers to the involuntary loss of control over bladder or bowel movements, often resulting in leaking urine or feces. It can occur due to various factors, such as weakened
Read more
Incontinence refers to the involuntary loss of control over bladder or bowel movements, often resulting in leaking urine or feces. It can occur due to various factors, such as weakened
Read more
posted: Mar. 15, 2024.
 Your hormones play a vital role in how you look and feel. When your hormones are out of balance, it affects everything from your skin to your moods. A hormonal
Read more
Your hormones play a vital role in how you look and feel. When your hormones are out of balance, it affects everything from your skin to your moods. A hormonal
Read more
posted: Mar. 01, 2024.
 An obstetrician/gynecologist, more commonly known as an OBGYN, is a vital part of your women’s healthcare team. An OBGYN can treat girls and women of all ages, from teen girls
Read more
An obstetrician/gynecologist, more commonly known as an OBGYN, is a vital part of your women’s healthcare team. An OBGYN can treat girls and women of all ages, from teen girls
Read more
posted: Feb. 26, 2024.
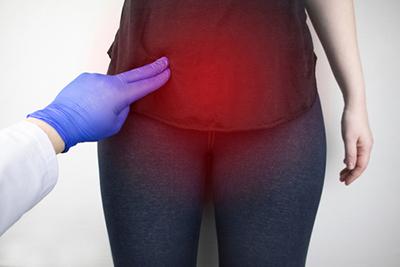 Abnormal uterine bleeding can be embarrassing. It can also be uncomfortable if it is associated with cramping and pain. Your OBGYN doctor is an expert at diagnosis and treatment of
Read more
Abnormal uterine bleeding can be embarrassing. It can also be uncomfortable if it is associated with cramping and pain. Your OBGYN doctor is an expert at diagnosis and treatment of
Read more
posted: Feb. 13, 2024.
 An OBGYN provides an important service for women who are looking to receive wellness exams. However, many younger women may not know what an OBGYN does or the value that
Read more
An OBGYN provides an important service for women who are looking to receive wellness exams. However, many younger women may not know what an OBGYN does or the value that
Read more
posted: Jan. 07, 2024.
 If you experience abnormal uterine bleeding, you may be wondering what you can do about it. These are some of the most frequently asked questions about abnormal uterine bleeding:
What Is
Read more
If you experience abnormal uterine bleeding, you may be wondering what you can do about it. These are some of the most frequently asked questions about abnormal uterine bleeding:
What Is
Read more
posted: Jan. 01, 2024.
 Menopause marks the natural cessation of menstrual cycles, typically occurring in your late 40s to early 50s. It heralds the end of fertility due to hormonal changes, leading to symptoms
Read more
Menopause marks the natural cessation of menstrual cycles, typically occurring in your late 40s to early 50s. It heralds the end of fertility due to hormonal changes, leading to symptoms
Read more
posted: Dec. 08, 2023.
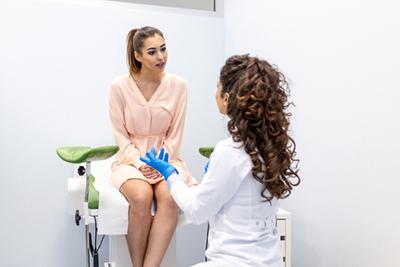 Women have specific needs that need to be overseen and taken care of. There are also many issues that can be treated or prevented easily with early detection. The best
Read more
Women have specific needs that need to be overseen and taken care of. There are also many issues that can be treated or prevented easily with early detection. The best
Read more
posted: Dec. 01, 2023.
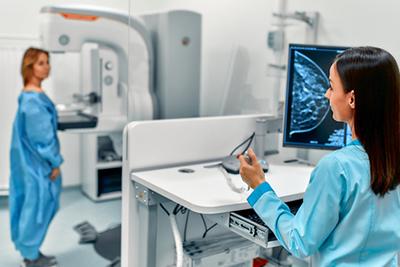 Breast cancer is a form of cancer that originates in the breasts and typically, you may feel a lump somewhere in the breast. Breast cancer is treatable, especially if it
Read more
Breast cancer is a form of cancer that originates in the breasts and typically, you may feel a lump somewhere in the breast. Breast cancer is treatable, especially if it
Read more
posted: Nov. 07, 2023.
 At least once each year, you make sure to visit your doctor as part of preventive healthcare. If you are a woman, it’s just as important to come in for
Read more
At least once each year, you make sure to visit your doctor as part of preventive healthcare. If you are a woman, it’s just as important to come in for
Read more
posted: Nov. 01, 2023.
 An obstetrics and gynecology doctor, commonly known as an OBGYN, is an important part of a woman’s healthcare team. The services an OBGYN provides can help ensure a woman’s reproductive
Read more
An obstetrics and gynecology doctor, commonly known as an OBGYN, is an important part of a woman’s healthcare team. The services an OBGYN provides can help ensure a woman’s reproductive
Read more
posted: Oct. 13, 2023.
 When it comes to women’s health, it’s important that you’re aware of the issues that you might face as you age. There are certain gynecological issues that can be associated
Read more
When it comes to women’s health, it’s important that you’re aware of the issues that you might face as you age. There are certain gynecological issues that can be associated
Read more
posted: Oct. 05, 2023.
 Getting pregnant doesn’t always happen quickly. Sometimes pregnancy can be difficult to achieve for many reasons. When you or your partner are having fertility issues, you need the help of
Read more
Getting pregnant doesn’t always happen quickly. Sometimes pregnancy can be difficult to achieve for many reasons. When you or your partner are having fertility issues, you need the help of
Read more
posted: Sep. 12, 2023.
 Women’s health is complex and there are certain needs that women have in their healthcare. It’s important to have a doctor who specializes in these needs and understands what you
Read more
Women’s health is complex and there are certain needs that women have in their healthcare. It’s important to have a doctor who specializes in these needs and understands what you
Read more
posted: Sep. 01, 2023.
 Irregular bleeding can be scary, especially if you don’t know what is causing it. Irregular bleeding can be occasional, or it can last for months, or even years. Our OBGYN
Read more
Irregular bleeding can be scary, especially if you don’t know what is causing it. Irregular bleeding can be occasional, or it can last for months, or even years. Our OBGYN
Read more